
In Lobamba, about twenty kilometers south of Eswatini’s capital Mbabane, more than six hundred residents lined up at Lombamba National Primary School for a mobile medical outreach.
Among them was an older woman leaning on two crutches. From a distance, she seemed to walk on four legs, yet every step still looked anchored to the ground. The short path from the school gate to the registration desk took her an hour. She was one of many poor and chronically ill residents in the area, and one of the 600-plus people who received care that day.
Public hospitals in Eswatini often run short of medicines and supplies, while private clinics are far beyond what most rural families can afford. Transport from outlying areas is difficult. Many people live for years with untreated illnesses and no access to basic drugs.
Since 2024, Tzu Chi’s mobile clinic team has been taking services into such communities. Doctors, nurses, physiotherapists, and a nutritionist travel together and provide consultations, basic tests, medication, and screening for breast cancer and HIV. The core team now numbers around twenty. What started as small outreaches serving just over a hundred people has grown. The clinic held at Lombamba on October 25, 2025, was the largest to date.
Order in a crowded schoolyard
On outreach day, the school courtyard became a busy triage area.
At the entrance, schoolchildren and Tzu Ching youth volunteers handled registration. Local volunteers guided patients to nursing students, who checked blood pressure, temperature, and blood sugar. Four classrooms were turned into consultation rooms for six doctors, with curtains to protect privacy and dignity.
The pharmacy classroom quickly became the most crowded space. The queue for medicine snaked out the door, and volunteers and police officers helped keep it moving. In a country where medicine is scarce and expensive, a small envelope of tablets can mean the difference between coping and collapse.

A few days earlier, overall coordinator Sharon Frazer (李后玉) and Pauline, a retired nurse from the United Kingdom with fifty years of experience, had gone from pharmacy to pharmacy in Mbabane to purchase enough medicines. Working with a budget of about 65 rand (roughly US$3.50) per patient, they assembled drugs for common and chronic conditions. Local businesses donated ingredients, and kitchen volunteers prepared about 900 meals so no one had to seek care on an empty stomach.
From one angle, the day felt like a success: hundreds of people were seen, screened, and given medication. From another, the scale of the need was sobering. So many residents had reached a point where untreated illness and malnutrition were everyday realities, and their calls for help barely carried beyond their own neighborhoods.
“Forgotten” children and urgent pain
At the physiotherapy tent, a boy in a wheelchair named Billy greeted visitors with a wide smile. He lives with cerebral palsy. His grandmother, Thulisile, had brought him, hoping for advice.
Billy is twelve. His limbs are as thin as twigs, his hands curled like hooks, his bones visibly displaced beneath taut skin. When his grandmother tried to adjust his legs, he could not form words; instead he cried out in pain, tears rolling down his cheeks.
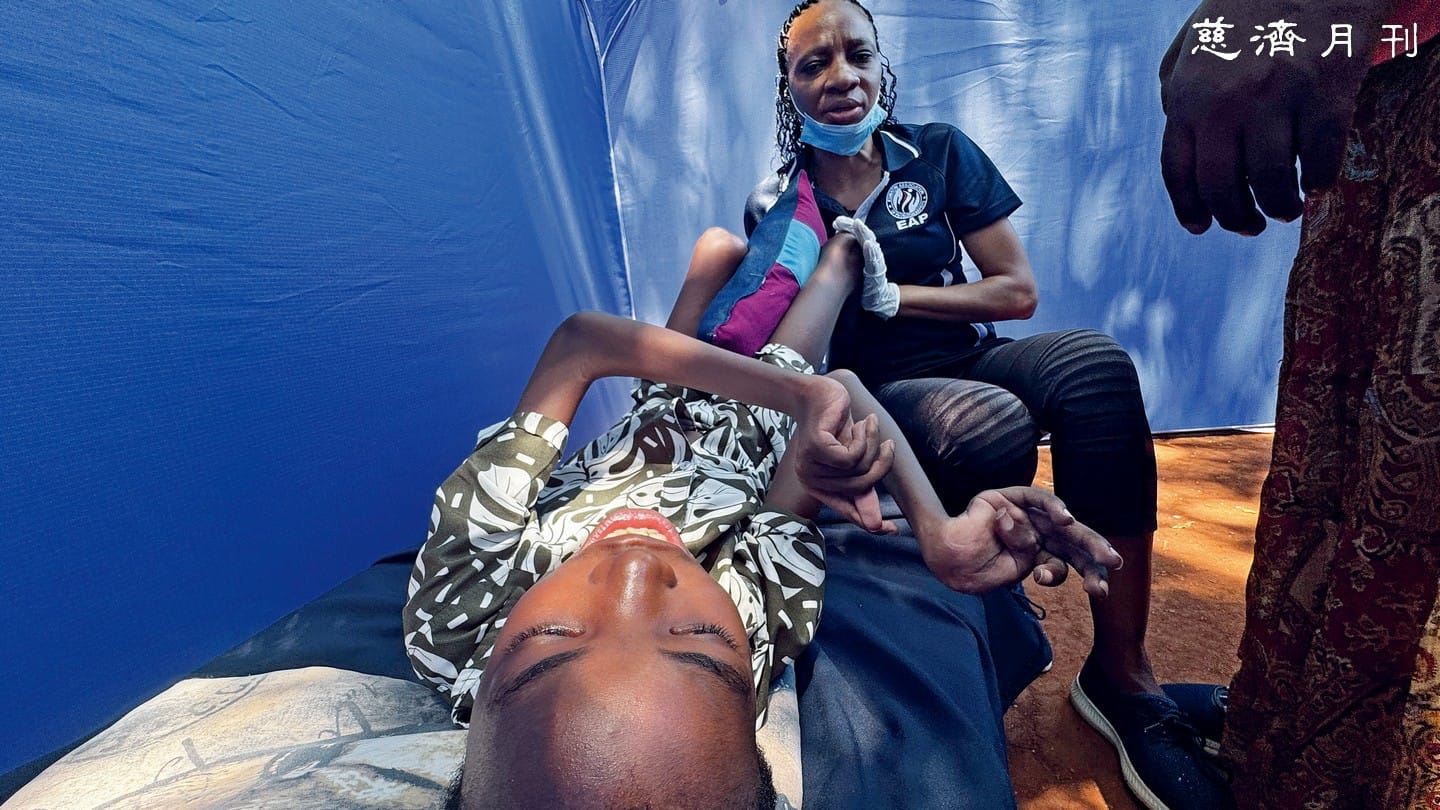
When she gently lifted his shirt, his ribs pushed out at strange angles. The sight was so unexpected that the visiting photographer paused. Billy’s body seemed to be “turning to stone”: contracted joints, contorted bones, and constant pain.
The physiotherapist did what she could—showing simple stretches and handling tips—but her assessment was blunt: Billy’s condition was already very serious. Years without proper medical support had taken their toll. Sharon and the team immediately noted the family’s address and arranged for a home visit, hoping to prevent another loss like an earlier case in Eswatini, a girl with cerebral palsy who had died soon after volunteers found her in 2012.
Thulisile supports a household of eleven—daughters and grandchildren—on irregular work and still buys diapers for Billy. For families like hers, regular physiotherapy and transport are simply out of reach. The mobile clinic was the first time in years that a trained professional had examined him.
“Please, can you take my children?”
Nearby, while Sharon was speaking with a malnourished mother, another woman drew close, her voice barely above a whisper. Her first words were not about pills or pain.
“Please, can you help me? Do you have a shelter? I have no home, no food, nothing… I can’t take care of my children.”
Her name was Siphesihle. She begged Sharon again and again to take her three children—a two‑year‑old son, a three‑year‑old daughter, and a six‑month‑old baby girl.
She had once had a job, but when her employer stopped paying wages, she lost it. With nowhere to live, she and the children drifted. At night, they secretly slept at a friend’s house; before dawn, they would slip away so the owner would not find them. For the children, early childhood had become a cycle of fleeing and hiding. Their mother’s despair had reached the point where handing them over to strangers felt like the only way out.
Siphesihle had no mobile phone and often no food. Sharon wrote down the friend’s phone number and added her to the home‑visit list.
Volunteers feared she might abandon the children. In the days after the outreach, they searched the surrounding communities until they finally found her. The three children were still by her side. Volunteers brought several months of food, easing at least the immediate pressure of hunger on the family.
A snapshot of Eswatini’s social crisis
According to UNICEF’s “Multiple Indicator Cluster Survey 2022–2023” for Eswatini, only 25 percent of children aged 0–17 live with both parents. The remaining 75 percent live with a single parent, grandparents or other relatives, or in institutions such as orphanages.
Those statistics took human form throughout the outreach: mothers on the verge of giving up their children, malnourished boys and girls, and young people with conditions like cerebral palsy left largely untreated.
Eswatini is known for having the world’s highest HIV prevalence. Yet a parallel health crisis—malnutrition—often receives less attention. At Lombamba, the degree of undernutrition among both children and adults startled many of the doctors.
Family physician Paulos S. Beshah noted that malnutrition and HIV share similar symptoms. Both weaken the immune system, leaving people vulnerable to infections that can quickly become fatal. In his words, “Even an ordinary cold can take a life.”
The principal of Lombamba National Primary School described another pattern: many teenagers become parents while still in school or soon after dropping out. Without guidance and education, they struggle to raise their children, and the next generation faces the same hardships.
Youth learning to serve
Yet in the same schoolyard, another current was quietly reshaping the community’s future.
More than a hundred local volunteers joined the mobile clinic, from young children to elders in their seventies. Many left home at four in the morning to be ready to serve by seven.

Under Sharon's patient guidance, a group of teenage volunteers learned to manage registration, direct patient flow, and support the medical team. When mistakes happened, she explained calmly instead of scolding, which built their confidence.
At a fundraising table, fourteen‑year‑old Bakahle introduced handmade cushions to the visiting photographer. Volunteers had sewn them stitch by stitch for patients to use while waiting or resting.
When asked why she chose to volunteer, she answered that people who came to “Tzu Chi” often arrived feeling lonely and unloved, but left feeling cared for. For her, the clinic was not only about medicine, but also about the experience of being seen.
Under a large tree, younger children wrote blessing cards by hand, each carrying simple words of encouragement for patients. The volunteers worked from morning until after sunset. In the pharmacy classroom, they kept packing medicines until the very last patient had received their free prescription. Only when all boxes of drugs and equipment were loaded back onto trucks did they relax.
One of the most energetic helpers was twelve‑year‑old Siyabonga. When a truck full of medicine crates pulled up, he jumped aboard without hesitation, hauling boxes under bright lights, sweat shining on his forehead.
By evening, when Sharon thanked everyone—saying the day’s success belonged to them—the courtyard echoed with young voices answering back.
Changing the course of a community
That day, hundreds of residents made their way to Lombamba National Primary School, some carrying babies on their backs, some supported by crutches, others guided by young volunteers.
They found not a hospital building, but a network of people: doctors who took time to listen, nurses and therapists who explained conditions and treatments, volunteers who offered meals, directions, or simply a steady arm on uneven ground.
For the school principal, the young volunteers’ dedication stood in stark contrast to stories of early pregnancy, alcohol use, and lost schooling that too often shape adolescence in the area. In the mobile clinic, those same teenagers were practicing responsibility, compassion, and discipline. Their example may influence classmates and neighbors in ways impossible to measure now.
The mobile clinic cannot solve Eswatini’s systemic challenges. Poverty and illness still reinforce each other, and many families remain at risk of falling through the cracks. But the outreach showed that when medical care comes closer to those who need it most—and when children and youth are invited to serve alongside professionals—another future begins to feel possible.
The steps toward that future may be slow, like the woman who needed an hour to reach the registration table. Yet she was not walking alone. Around her, and around families like Billy’s and Siphesihle’s, new circles of support are quietly forming.
Written by Dai‑Rong Lin (林岱融)



